With the end of the academic year, I have gratefully begun a 16-month sabbatical. A sabbatical leave is an extraordinary perk within academic life, particularly when one has grant funding to “buy-out” a full academic year (versus a one-semester sabbatical that typically comes along every seven years in a professor’s life). The word “Sabbatical” is defined by Merriam-Webster as: “…a period of time during which someone does not work at his or her regular job and can rest, travel, or do research.” The word traces back to the Hebrew word, Shabbat, which means rest. And after a fairly stressful and extraordinary year of managing pandemic life and doing everything from teaching, training, conducting research, seeing patients, and socializing online, the idea of rest is compelling. Yet, as we slowly emerge from our pandemic nightmare, there is a burgeoning energy that wells up with the prospect of “getting back to normal” and, for me, the opportunities that arise from not doing my regular job for many months.
I will thus endeavor to rest during sabbatical and re-approach traveling to give face-to-face talks, visit with friends and research collaborators, and of course, focus on research and writing. As with previous sabbaticals, I will use this amazing gift of scholarly time from the day job to write a book, in this case, the 3rd edition of my Guilford Press book, <em>Managing Suicidal Risk: A Collaborative Approach</em>. With my book contract now freshly signed, the words and ideas that have been accumulating in my head over the past several years will finally be transformed into written text for what will be the final edition of a 3-part series on the CAMS Framework®. While it may not be my final book, it nevertheless feels like closing a certain loop of a 30+ year endeavor. Consequently, I anticipate blogging about various intellectual reflections related to various sabbatical-inspired projects in the coming months.
This line of musing now leads me to reflect on the word “distress.” As per Merriam-Webster, distress is a multi-purpose word that can be used as a noun, verb, and adjective. For the present discourse, I am drawing from each of these uses in that they emphasize variants of the following: pain, suffering, a painful situation, worry, troubled, upset, great strain, difficulties, a state of danger, or desperate need.
<h2>Distress and COVID-19</h2>
Over the past year, for millions of people worldwide, the distress of COVID-19 has been breathtaking; and tragically, for far too many cases, I mean this literally. Here in the United States, we have lost more than half a million Americans to COVID-19. And, while the genius of scientists creating life-saving vaccines is a marvel, the distress that so many have endured—in all its forms—is like nothing we have ever experienced.
<h2>The Difference Between “Stress” and “Distress”</h2>
That said, when any of us think about contemporary modern-day life, certainly we all must acknowledge the experience of stress. Indeed, even while on vacation (or a scholarly sabbatical), wherein we do our best to rest, recoup, unwind, and de-stress, the reality is that we still encounter various stressors within our daily lives. Stress is simply a reality of life, and while it may strain our sense of well-being, many of us are generally able to manage it and settle ourselves back down. But for some people, particularly people who are suicidal, stressors are a constant and may transmute into a state of seemingly constant distress. To say the least, being in a pervasive state of distress is miserable. For some, intense distress can become so utterly insufferable that thoughts of suicide, dangling the possibility of relief from misery, can become persuasive and compelling—what has been referred to as the <em>siren song of suicide</em>.
<h2>CAMS Reduces Distress and Promotes Distress Tolerance</h2>
It is with these considerations in mind that I finally get to the main point of this blog. Among the many exciting findings of the recent <a href=”https://cams-care.com/resources/blog/cams-meta-analysis-intervention-for-suicidal-ideation/” target=”_blank"”>Swift et al. meta-analysis of nine CAMS clinical trials</a>, one finding is often overlooked, even by me. It is the robust finding that has been seen across a number of CAMS clinical trials. CAMS reliably and significantly reduces distress in comparison to other treatments. This finding has been replicated across various CAMS trials and is one of the most consistent clinical outcomes of receiving CAMS. Across clinical trials, the construct of “general distress” has been measured by the Outcome Questionnaire-45 (OQ-45), the Brief Symptom Inventory (BSI), and the WHO Disability Assessment Schedule (WHO-DAS). Within the clinical trials research of CAMS, in which I have been involved, we have primarily used the well-constructed OQ-45 as our measure of general distress. The SD sub-scale of the OQ measures symptom distress as an overall index of intrapsychic functioning with an emphasis on depression and anxiety. The BSI and WHO-DAS similarly describe the severity of symptoms/illness and assess general health and disability, respectively. In other words, beyond significantly and reliably reducing suicidal ideation and hopelessness, CAMS also reliably and significantly reduces the profound distress which fundamentally shapes and defines unbearable suicidal misery. Perhaps part of the “secret sauce” of what makes CAMS work for people who are suicidal is moving omnipresent and pervasive distress that feeds suicidal thinking to a level of tolerable and more manageable stress. Maybe CAMS even helps the person who is suicidal with the ability to rest, recoup, unwind, and de-stress from previously seemingly endurable psychological pain, which is at the heart of most suicidal states. Certainly, the clinical effect is not equivalent to a psychological vacation—let alone a sabbatical leave. But perhaps it enables the patient to regroup and catch their psychological breath? And with life-giving breath, the potential for hope can grow, and a life worth living might be possible?
<h2>Distress Reduction and Tolerance Can Change Patients’ Lives</h2>
I thus eagerly turn my attention to book-writing and the abundant possibilities of sabbatical. As I reflect on my blessings, the gift of having manageable stressors comes to mind. To be sure, my life, just like anyone else’s, has many stressors—worries related to family and friends, our contentious and fragile democracy, unconscionable racism, horrible treatment of marginalized populations, along with hate and interpersonal meanness that has become ubiquitous within our daily lives. Will I get the book done on time? Will this next crucial grant come through? What will be the findings of these current RCTs? What will it be like to travel abroad and eat in a restaurant again? What will it be like to see dear friends and colleagues who have been relegated to 2-dimensional images on my computer screen? Yes, of course, all these things and more can stress me out. But within each of these stressors, there are also potentials for great outcomes, historic breakthroughs, kindnesses, and acts of goodness. Books will get written, grants will come through (or not), and RCTs will be completed and published. Travel and restaurant dining will once again become routine; dear friends and colleagues will be seen and warmly embraced. In short, my life stressors are usually manageable and worth managing. However, unlike my patients and research participants who are suicidal, my stress has never become distress that permeates every dimension of life so that suicide becomes an obvious and compelling solution. It is a remarkable clinical and research accomplishment that CAMS reliably helps such people reduce their distress such that suicide is no longer their most compelling solution. Henceforth, I will thus endeavor not to overlook this finding as one key ingredient for successfully treating highly distressed people who entertain serious thoughts of suicide.
* * * * *
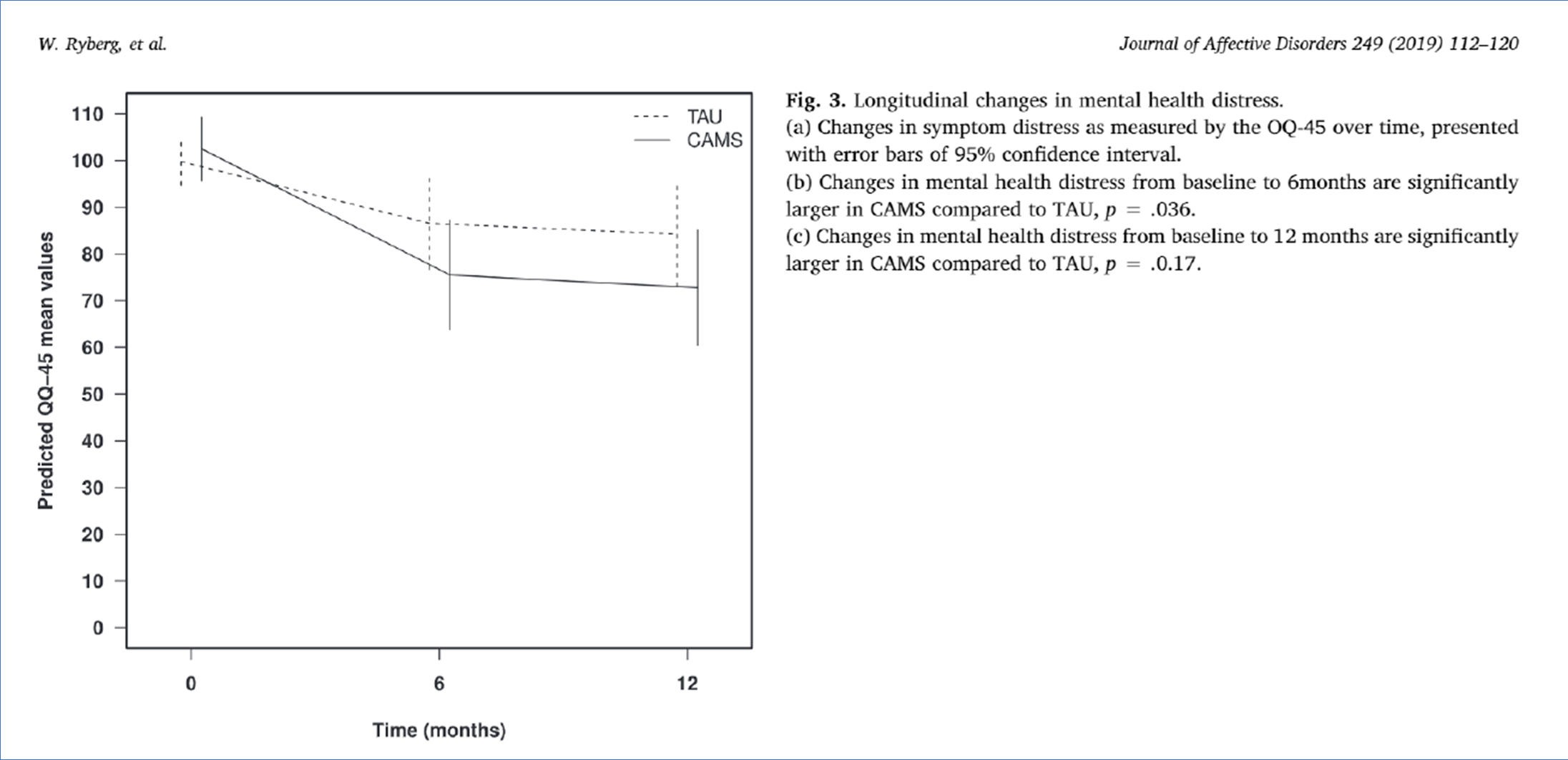
From Ryberg et al.’s (2019) Norwegian randomized controlled trial of CAMS vs. Treatment as Usual.
About CAMS-care
At CAMS-care, we offer suicide assessment and prevention training, consulting, and resources. For more information on CAMS, please contact us.
